Healthcare mergers and acquisitions reshape the medical landscape in Hermosa Beach and beyond. These transactions involve complex legal, financial, and regulatory considerations that can make or break a deal.
At Pierview Law, we’ve guided healthcare organizations through countless M&A processes. This guide walks you through the essential steps to protect your interests and achieve a successful transaction.
What Drives Healthcare Organizations to Merge
Financial Distress as a Primary Motivator
Healthcare mergers and acquisitions reshape the medical landscape in Hermosa Beach and beyond. These transactions stem from concrete financial and operational pressures rather than abstract strategic ideals. In 2025, 43 percent of healthcare M&A transactions involved a financially distressed party, according to Kaufman Hall’s end-of-year report. This statistic reveals the harsh reality: many organizations cannot survive independently. Rising costs, shrinking reimbursement rates, and workforce shortages push healthcare providers toward consolidation.
Tariffs, uncertainty around Medicare and Medicaid reimbursement, and the escalating cost of care accelerated deal activity throughout 2025 and into 2026. Organizations in Hermosa Beach and across Los Angeles County face these same pressures.
When a healthcare provider approaches you about a potential merger or acquisition, financial distress often sits beneath the surface, even if leadership frames the transaction as a growth opportunity. Understanding this reality helps you evaluate whether the deal truly serves your organization’s long-term interests or simply postpones inevitable decline under new ownership.
Mergers Versus Acquisitions: Structural Differences
A merger differs fundamentally from an acquisition in both legal structure and execution speed. In a merger, two organizations combine to form a new entity with shared ownership and governance. An acquisition occurs when one organization purchases another and absorbs it entirely. The distinction matters legally and financially because mergers typically involve more complex negotiations around ownership percentages, board composition, and leadership roles. Acquisitions move faster because the acquiring organization maintains control and decision-making authority.
From a regulatory standpoint, both structures trigger California’s expanded oversight rules. As of January 1, 2026, the California Office of Health Care Affordability requires 90-day advance notice for material asset transactions involving noticing entities such as management services organizations, private equity groups, and hedge funds. This means your M&A timeline must account for mandatory regulatory review periods that could extend deal closure by months.
California’s Tightened Regulatory Framework
The regulatory framework in California has tightened considerably. AB 1415 and SB 351, passed in October 2025, fundamentally reshape how private equity and hedge funds can structure healthcare deals. SB 351 prohibits investors from interfering with physicians’ and dentists’ independent professional judgment, including decisions about hiring, firing, diagnostic testing, and patient volume thresholds. Contracts that violate these restrictions become void and unenforceable.
This matters directly for Hermosa Beach healthcare providers considering partnerships with outside investors. You cannot accept investor control over clinical decisions, billing practices, or medical equipment selection. The California Attorney General enforces SB 351 and can seek injunctive relief, attorneys’ fees, and other remedies. Non-compete and non-disparagement provisions in management services agreements face restrictions unless they protect genuinely confidential business information in a sale.
Compliance Timing and Strategic Planning
These regulatory constraints eliminate entire deal structures that would have worked under prior law. Organizations that delay compliance work until after signing a letter of intent face substantial renegotiation costs and timeline extensions. Beginning regulatory and CPOM compliance reviews immediately positions your organization to identify structural barriers early and negotiate more effectively with potential partners.
The financial pressures driving healthcare consolidation show no signs of abating. As you evaluate whether M&A makes sense for your organization, the legal and regulatory landscape demands attention from day one. Understanding what financial and operational factors motivate potential partners-and what regulatory boundaries constrain deal structures-sets the foundation for sound decision-making. The next phase of your M&A journey requires rigorous financial and operational evaluation to determine whether a proposed transaction actually strengthens your organization or simply transfers control to a stronger party.
What Financial and Operational Data Reveals About Deal Risk
Audited Statements and Hidden Liabilities
Financial statements tell the story of whether a healthcare organization can survive independently or whether distress masks itself behind optimistic projections. Demand audited financial statements for the past three years, not unaudited drafts or management estimates. Audited statements follow GAAP standards and provide credible baseline data for revenue trends, expense patterns, and cash flow stability. Review audit reports and management letters carefully-auditors flag control weaknesses, compliance gaps, and financial risks that management might downplay.
A management letter noting significant deficiencies in billing controls or revenue cycle processes signals operational fragility that extends beyond balance sheet figures. Analyze debt instruments line by line, including covenants that restrict operations or trigger default upon change of control. Many healthcare providers face hidden debt acceleration clauses that activate during M&A, creating surprise liabilities at closing. Check liens against assets, inventory utilization statistics, and accounts receivable aging to gauge whether the organization’s stated financial position matches operational reality. A practice showing strong paper profits but deteriorating collections indicates revenue quality problems that persist after acquisition.
Clinical Outcomes and Regulatory Compliance Status
Clinical outcomes data and patient satisfaction metrics matter as much as financial statements because they predict post-merger integration costs and revenue retention. Request The Joint Commission accreditation reports, state Department of Health inspection records, and CMS quality reporting data for the past two years. Organizations with survey deficiencies face remediation costs that acquirers typically absorb after closing.
Verify licensing and credentialing status for all physicians and advanced practitioners-incomplete or lapsed credentials create liability exposure and disrupt patient care continuity. Review managed care contracts to understand payer mix, reimbursement rates, and contract terms that survive or terminate upon change of control. Some payers include provisions allowing termination if ownership changes materially, which means acquisition could immediately reduce revenue by 15 to 25 percent.

Internal Controls and Compliance Assessment
Establish an internal financial control assessment through review of accounts payable processes, payroll administration, and fixed asset tracking. Organizations with weak controls frequently hide compliance violations or billing errors that surface during regulatory review. Assemble a cross-functional team early that includes regulatory counsel, compliance personnel, and financial advisors to map CPOM risk, assess MSO structure compliance, and identify which contracts require renegotiation under AB 1415 and SB 351 (these parallel work streams prevent surprises after letter of intent signing and position you to negotiate more effectively with potential acquirers).
The 90-day OHCA notice period under AB 1415 becomes manageable only when financial and operational due diligence occurs simultaneously with legal and regulatory assessment, not sequentially. This integrated approach exposes structural barriers early and clarifies which deal terms require modification to satisfy California’s tightened restrictions on investor control and clinical independence. Once you understand your financial position and operational vulnerabilities, the next phase focuses on the legal agreements and regulatory pathways that govern how transactions actually close.
Navigating Legal and Regulatory Hurdles
Antitrust Analysis Shapes Your Competitive Position
California’s regulatory environment now demands immediate antitrust analysis before you enter serious negotiations. The California Attorney General enforces both AB 1415 and SB 351, meaning state officials actively scrutinize healthcare transactions for competitive harm and improper investor control. OHCA cannot independently block a deal, but it refers objectionable transactions to the Attorney General for potential antitrust challenge, creating a formal enforcement pathway that extends deal timelines unpredictably.
When you file your 90-day notice with OHCA under AB 1415, regulators assess whether the transaction reduces competition in your local market, affects healthcare affordability, or disrupts workforce stability. For Hermosa Beach organizations, this means analyzing your competitive position against other providers in Los Angeles County before approaching potential partners. A merger that strengthens your bargaining power with payers may trigger antitrust concerns if it reduces patient choice in your service area.
Organizations like Hartford HealthCare, which invested over $225 million in two Prospect hospitals after acquisition, faced scrutiny precisely because consolidation affects pricing power and patient access. The DOJ required UnitedHealth Group to divest at least 128 home health and hospice facilities after its Amedisys acquisition, demonstrating that regulators will dismantle deals that concentrate market power excessively. Your antitrust analysis must map patient flows, payer relationships, and competitor locations within a realistic service radius before you commit to negotiating terms.
Contract Review Under SB 351 and AB 1415
Contract renegotiation under SB 351 and AB 1415 requirements creates substantial execution risk if you delay compliance work. Every management services agreement, physician employment contract, and payer arrangement requires legal review to identify provisions that become void under the new restrictions on investor control over clinical decisions, billing practices, and equipment selection. Non-compete clauses in management agreements face particular scrutiny unless they genuinely protect confidential business information in a transaction context.
Establish a centralized contract management system documenting all material agreements, expiration dates, and renewal triggers before you enter due diligence to prevent surprises during integration. This system allows you to track which contracts require renegotiation and which ones survive the transaction intact. Organizations that postpone this work until after signing a letter of intent face substantial renegotiation costs and timeline extensions.
Licensing, Credentialing, and Regulatory Verification
Licensing and credentialing verification must confirm that all physicians, dentists, and advanced practitioners hold current, unrestricted licenses and that credentials verification organizations have processed all applications successfully. Missing or lapsed credentials create liability exposure that acquirers inherit immediately upon closing. Request verification reports from your state medical board and The Joint Commission to confirm compliance status across your entire clinical workforce.
This verification process should occur simultaneously with antitrust analysis and contract review, not sequentially. Parallel work streams prevent surprises after letter of intent signing and position you to negotiate more effectively with potential acquirers. Organizations that complete this assessment early identify which staff members require credential updates before closing and which regulatory approvals take longest to obtain.
Integration Planning and Sequencing
The integration planning process should address clinical program design, physician alignment, and governance structure last because these elements depend on resolving financial, operational, and regulatory issues first. AHA Market Scan Trailblazers research on post-merger integration demonstrates that hospital systems typically require 1 to 2 years to complete integration, with people-focused functions and operational systems like human resources, finance, and revenue cycle integrated earliest to maintain organizational stability.
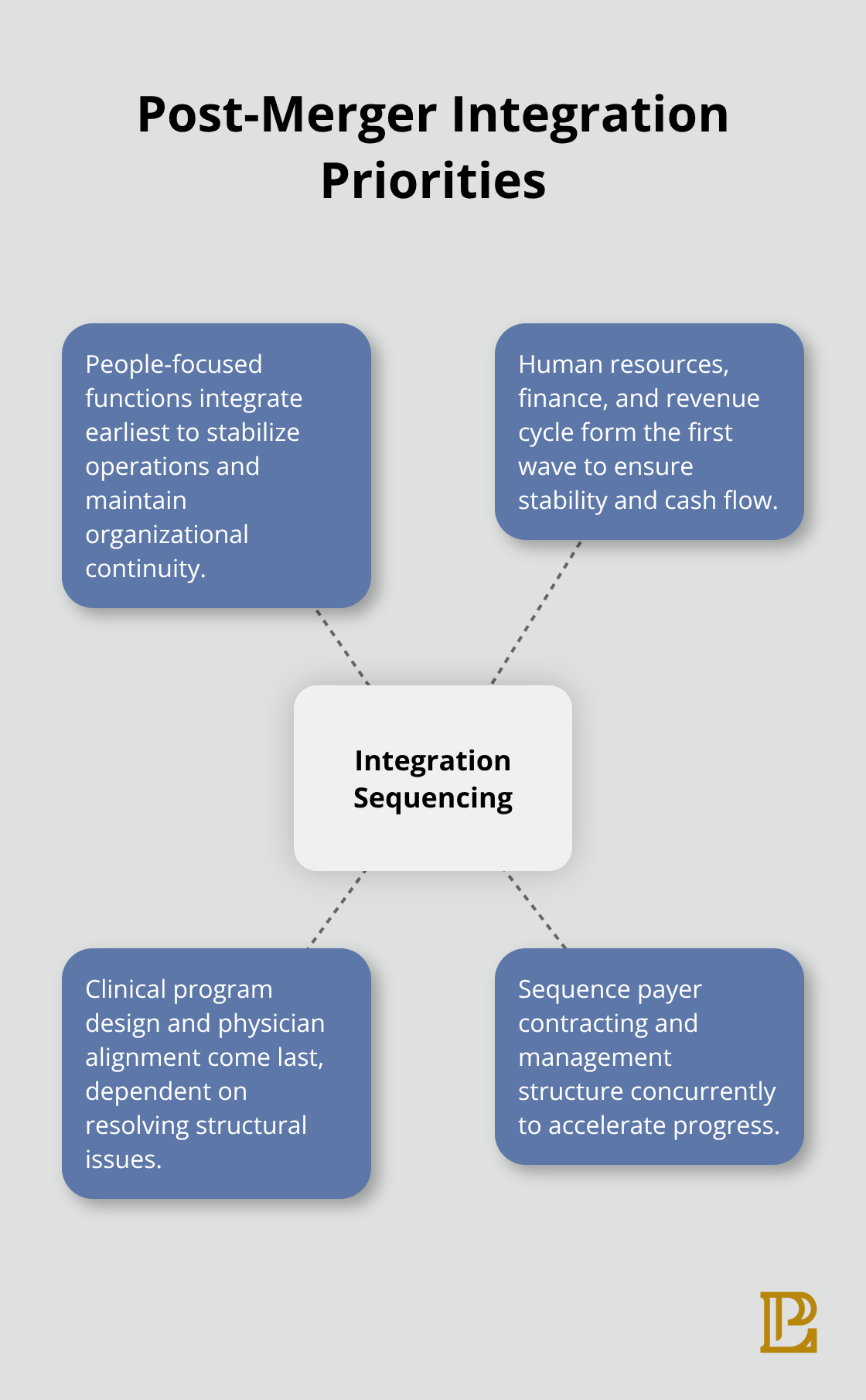
Shorter timelines sustain momentum and signal a finite path to completion for employees and clinical staff. Your integration road map should sequence activities correctly, with payer contracting and management structure addressed concurrently rather than sequentially to accelerate progress. This antitrust analysis must occur simultaneously with CPOM and licensing review to create an integrated regulatory, legal, and operational assessment that identifies structural barriers early and positions you for successful negotiations with potential partners or acquirers.
Final Thoughts
Healthcare mergers and acquisitions succeed when organizations address financial, operational, legal, and regulatory issues simultaneously rather than sequentially. The 2025 and 2026 landscape demands this integrated approach because California’s AB 1415 and SB 351 restrictions eliminate deal structures that worked under prior law. Organizations that delay compliance work until after signing a letter of intent face substantial renegotiation costs, timeline extensions, and potential deal failure.
Three parallel work streams must start from day one. Conduct rigorous financial and operational due diligence that examines audited statements, clinical outcomes, managed care contracts, and internal controls to identify hidden liabilities before they become your problem, assess regulatory compliance simultaneously by reviewing CPOM restrictions and contract provisions that violate SB 351, and map your competitive position and antitrust exposure before approaching potential partners so you understand whether consolidation strengthens your bargaining power or triggers regulatory objections. Post-merger success depends on clear integration planning that sequences activities correctly, with people-focused functions like human resources, finance, and revenue cycle integrating earliest to maintain organizational stability while clinical program design and physician alignment come last because they depend on resolving structural and operational issues first.
The regulatory environment in California will continue tightening, so monitor enforcement actions by the California Attorney General and guidance from OHCA to stay informed about how regulators interpret AB 1415 and SB 351. If you operate a healthcare practice or organization in Hermosa Beach or Los Angeles County and need guidance on health care mergers and acquisitions strategy, contact Pierview Law to discuss your specific situation.

